Nail Care
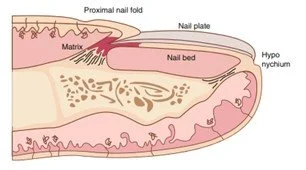
Nails are made of keratin the same protein that our hair is made of, not calcium as is often believed. The nail plate (the bit that we can see) is made of fully keratinised dead cells and the nail matrix at the base of the nail continuously produces cells to form the nail plate (Piraccini, 2014). Nail shape is determined partly by the size and shape of the phalanges (toe bones). Fingernails grow approximately 3 times as quickly as toenails (Haneke, 2014).
Common nail problems seen by podiatrists can include fungal infections, changes in shape or colour and ingrown toenails.
[Image source: Piraccini, 2014]
Ingrown Toenail
Ingrown toenails occur when the edge of the nail plate pushes into the surrounding skin, causing a wound and inflammation. Teenagers and people in their twenties (particularly males) are most likely to develop an ingrown toenail. This is thought to be due to increased sweating and taking part in sports, as well as growth spurts causing shoes too become too small. Nails thicken as we age, so are less likely to have sharp edges, reducing the risk of developing an ingrown nail although they can still occur following injury (Khunger and Kandhari, 2012). If left untreated, ingrown toenails can become infected and very painful, as well as unsightly.
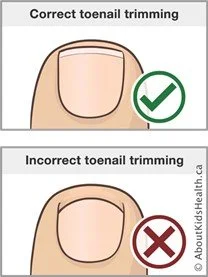
Ingrown toenails can be prevented by wearing the correct size shoes; there should be 1cm between the end of your longest toe and the end of the shoe. There should also be enough width for your foot. Cutting your toenails correctly is also important. Nails should be cut straight across, leaving a small amount of white. Cutting down the sides of the nail can leave a small bump or spike of nail which pushes into the skin as the nail grows. As tempting as it may be to try and cut the nail back further to resolve this, it is better to see a podiatrist who has the equipment and experience to do so.
The wound created by an ingrown nail can become infected. This is easily treated with antibiotics, however these will not get rid of the ingrown toenail. The only effective treatment is removal of the piece of nail that is causing the problem. This may involve a podiatrist cutting the nail back so that it can regrow normally or by having a minor surgical procedure to permanently remove the edge of or the whole nail. Your podiatrist will discuss the most appropriate course of treatment at your appointment. It is better to seek treatment sooner rather than later, especially if you have diabetes, circulation problems or smoke.
If you have an ingrown toenail which is bleeding or leaking fluid or pus, it is important to keep it clean to reduce the risk of infection. You can clean the toe by bathing it for a couple of minutes in salt water (boiled water that has cooled to a comfortable temperature with a pinch of table salt in it). Leave the toe to dry naturally - don’t be tempted to use cotton wool, tissue or towels to clean it further as this can introduce fibres and bacteria – then cover it with a plaster. Change the dressing every couple of days, or sooner if it gets wet, dirty or fluid from the toe leaks through.
Babies can also develop ingrown toenails. This is because their nails are very sharp, and they outgrow their Babygros. The pressure of the tight Babygro on their toes can cause a nail to push into the skin and cause a wound. These are easily managed by washing the wound with salt water and covering with a plaster to reduce the risk of infection. Toenails can be cut straight across if they are long, then either move to a larger size of Babygro or sock or cut the feet off the current Babygro to allow the toes some space. GPs can prescribe antibiotics if there is redness, pus or swelling of the toe, but it is unusual for any further treatment to be required.
Fungal nail infections
Fungal nail infections can cause a nail to change colour, thickness and texture. They are caused by fungi which live on our skin naturally. A nearby overgrowth (like athlete’s foot) or damage to a nail or the surrounding tissue can allow the fungi to start to grow in the nail matrix, nail bed or hyponychium, causing the change in the nail (Piraccini and Alessandrini, 2015). Some people are more susceptible to skin fungal overgrowths than others.
GPs sometimes ask for nail clippings to confirm the diagnosis of a fungal nail infection, however these often do not grow anything because there are no live cells in the sample.
A fungal nail infection can be treated with treatments available from the chemist, such as lacquers, or with a course of tablets from your GP. The treatment will depend on the type of infection you have. Effective treatment usually takes 3-6 months due to the slow growth rate of toenails and relies on the treatment soaking into the infected tissue. Natural remedies for fungal nail infections, such as cider vinegar, tea tree oil or Vicks Vaporub may be suggested elsewhere on the internet. There is no evidence that cider vinegar will treat a fungal nail infection (Rare and Care, 2017). There is some limited evidence to support the use of tea tree oil, however it can cause skin irritation and photosensitivity so speaking to a health professional first would be advisable (Nickles et al, 2022).
Wearing a clean pair of socks every day and treating shoes can reduce the risk of reinfection. Taking the insoles out of trainers, opening the shoes up and allowing them to air (putting them in the sun to dry is even better) helps with shoe hygiene. Treating shoes with antifungal spray or powder can also help prevent recurrence.
Other Concerns
There are plenty of other problems which affect toenails, however I’m trying to keep this short! If you have concerns about your toenails, speak to a podiatrist or your GP who may be able to provide diagnosis and advice or treatment. Taking pictures of your affected toe(s) every few days or each week can show how things have changed and can be particularly useful to health professionals when making a diagnosis. If the problem is painful or rapidly getting worse, do not delay in seeking treatment particularly if you have diabetes or a condition causing poor arterial circulation.
References
1. Haneke, E., 2014. Anatomy, biology, physiology and basic pathology of the nail organ. Hautarzt, 65(4), pp.282-290.
2. Khunger, N. and Kandhari, R., 2012. Ingrown toenails. Indian journal of dermatology, venereology and leprology, 78, p.279.
3. Nickles, M.A., Lio, P.A. and Mervak, J.E., 2022. Complementary and Alternative Therapies for Onychomycosis: A Systematic Review of the Clinical Evidence. Skin Appendage Disorders, 8(4), pp.269-279.
4. Piraccini, B.M. and Alessandrini, A., 2015. Onychomycosis: a review. Journal of Fungi, 1(1), pp.30-43.
5. Piraccini, B.M. and Piraccini, B.M., 2014. Nail anatomy and physiology for the clinician. Nail Disorders: A Practical Guide to Diagnosis and Management, pp.1-6.
6. Rare, T.F.I. and Care, T., 2017. Myths in Treating Onychomycosis. Onychomycosis, p.215.